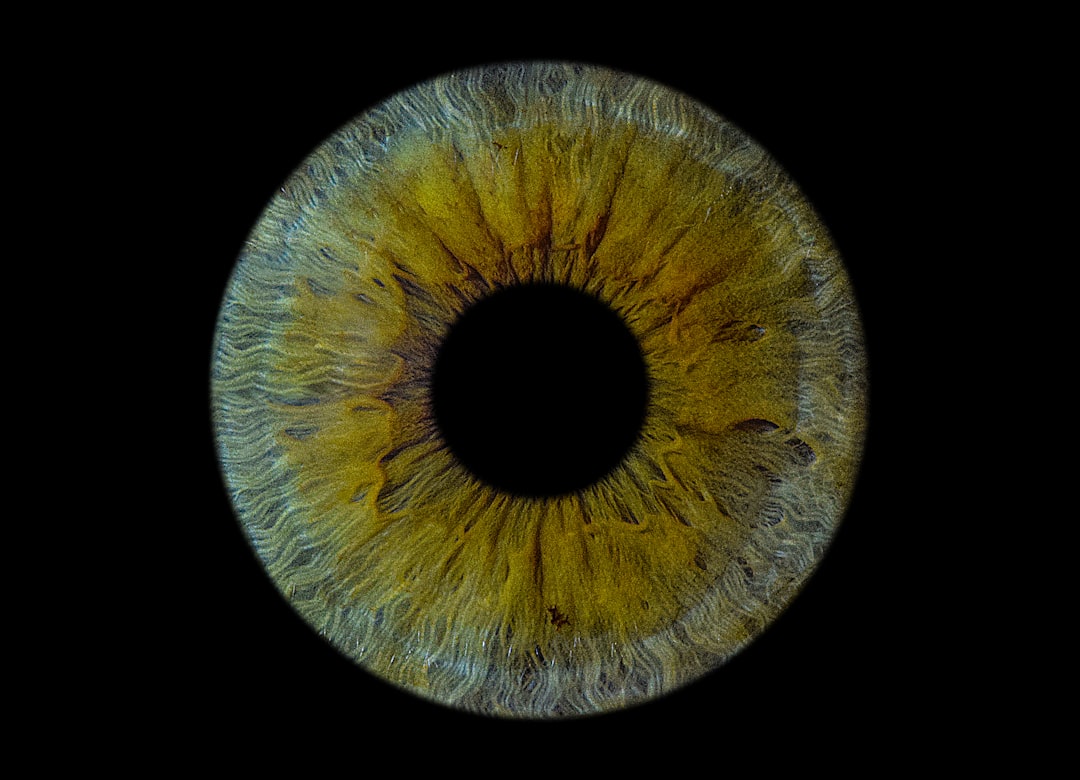
You’ve likely heard that being significantly nearsighted, or highly myopic, increases your risk of certain eye conditions. One of the most serious is retinal detachment. Understanding this link is crucial for your eye health, allowing you to take proactive steps and recognize potential warning signs. This article aims to demystify the connection, explain why you’re at a higher risk, and what you can and should do about it.
Before delving into the specifics of retinal detachment and myopia, it’s essential to have a basic grasp of your eye’s structure. Think of your eye as a complex biological camera, where the image you see is captured and transmitted to your brain.
The Cornea and Lens: Focusing Power
Your cornea, the transparent front surface of your eye, and the lens behind your iris, are primarily responsible for bending (refracting) light. Their combined power focuses light precisely onto the retina. In a properly functioning eye, this focused light creates a sharp image.
The Retina: The Light-Sensitive Layer
At the back of your eye lies the retina, a thin, light-sensitive tissue. It’s composed of millions of specialized cells called photoreceptors – rods and cones – which convert light into electrical signals. These signals are then processed and transmitted to your brain via the optic nerve, where they are interpreted as vision. The retina is analogous to the film or sensor in a camera.
The Vitreous Humor: Maintaining Shape
The vast majority of the space within your eyeball is filled with a clear, gel-like substance called the vitreous humor. This gel helps to maintain the eye’s spherical shape, providing structural support. It’s connected to the retina, particularly at its periphery.
Retinal detachment is a serious condition that can be particularly associated with high myopia, as individuals with severe nearsightedness are at an increased risk for this sight-threatening issue. For a deeper understanding of the relationship between high myopia and retinal detachment, you can explore this informative article that discusses the underlying mechanisms and preventive measures. To read more, visit this article.
Defining High Myopia: More Than Just Needing Glasses
Myopia, or nearsightedness, occurs when your eye focuses light in front of the retina instead of directly on it. This usually happens because either your eyeball is too long, or your cornea and lens are too powerful in their refractive ability.
The Refractive Error Spectrum
Nearsightedness exists on a spectrum. Mild myopia might require glasses or contact lenses for specific activities like driving or reading a whiteboard. Moderate myopia requires correction for most daily tasks. High myopia, however, refers to a more significant degree of nearsightedness.
Quantifying High Myopia
Clinically, high myopia is generally defined as a refractive error of -6.00 diopters or more. Diopters are the units of measurement for the power of a lens. A higher negative number indicates greater nearsightedness. If your prescription falls into this range, you are considered highly myopic.
The Ocular Elongation Factor
In most cases of high myopia, the primary cause is axial elongation. This means your eyeball has grown excessively long. This stretching weakens and thins the various layers of the eye, including the retina. Imagine stretching a rubber balloon; the material becomes thinner and more susceptible to tearing.
The Biomechanical Link: How Stretched Eyes Lead to Retinal Problems
The elongation of the eyeball in high myopia has direct implications for the structural integrity of your retina. This is where the increased risk of retinal detachment truly begins.
Retinal Stretch and Thinning
As your eyeball elongates, the retina, which lines the back of the eye, is stretched. This stretching can cause the retinal tissue to become thinner and more fragile. Imagine pulling a thin sheet of paper; it becomes more prone to tearing. This thinning is not uniform and can create areas of weakness.
Posterior Vitreous Detachment (PVD): A Common Precursor
The vitreous humor, while generally stable, can undergo changes over time. In older age, or in eyes that have undergone significant elongation, the vitreous can liquefy and begin to shrink. This shrinkage can cause the vitreous to pull away from the retina, a process known as posterior vitreous detachment (PVD). While PVD is a common age-related change and not necessarily pathological on its own, in highly myopic eyes, this pulling force can be more significant due to the vitreous’s attachment to the thinned retina.
Tractional Forces and Retinal Tears
In some cases, the vitreous may not detach cleanly. If there are areas of adhesion between the vitreous and the weakened retina, the shrinking vitreous can exert tractional forces. These forces can pull on the retina, potentially leading to the formation of small tears or holes in the retinal tissue. These tears are the gateway to retinal detachment.
The “Lattice Degeneration” Phenomenon
Highly myopic eyes are also more prone to developing a condition called lattice degeneration. This refers to areas of thinning and damage in the peripheral retina, often with a criss-cross pattern of white or yellowish lines. These areas are particularly vulnerable to tearing because they are already compromised. The weakened blood vessels within these degenerated areas can also be a factor in the development of tears.
Retinal Detachment: The Serious Complication You Need to Understand
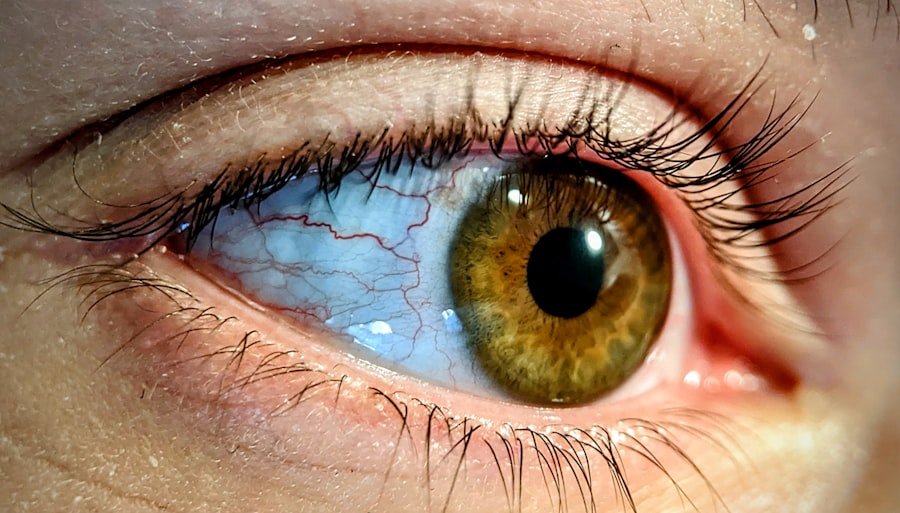
Retinal detachment occurs when the retina separates from the underlying supportive tissue, known as the retinal pigment epithelium (RPE). This separation deprives the photoreceptor cells of oxygen and nutrients, leading to vision loss if not treated promptly.
The Different Types of Retinal Detachment
Understanding the mechanisms by which the retina detaches is important for appreciating the link with high myopia.
Rhegmatogenous Retinal Detachment: The Most Common Type
This is the most frequent form of retinal detachment, and it’s directly linked to the retinal tears discussed previously. When a tear forms in the retina, liquid vitreous humor can seep through the tear, accumulating behind the retina. This fluid pushes the retina away from the RPE, causing it to detach. The presence of tears caused by tractional forces or lattice degeneration in highly myopic eyes makes them particularly susceptible to this type of detachment.
Tractional Retinal Detachment
While less common in general, tractional retinal detachment can occur in eyes with advanced myopic changes or other conditions like diabetic retinopathy. In this scenario, scar tissue on the surface of the retina contracts, pulling the retina away from the RPE. While elongated eyeballs themselves don’t directly cause scar tissue formation, the altered biomechanics and potential for micro-damage in high myopia can create an environment where such scarring is more likely to develop, especially if there are other co-existing factors.
Exudative Retinal Detachment
This type of detachment is caused by the accumulation of fluid beneath the retina, but without a tear. This fluid can originate from conditions that cause inflammation or leakage from blood vessels in the choroid (the vascular layer beneath the RPE) or the RPE itself. While not directly caused by the axial elongation of myopia, certain inflammatory conditions that might be more prevalent or have a different presentation in individuals with high myopia could contribute to exudative detachments. However, rhegmatogenous detachment due to retinal tears remains the primary concern for highly myopic individuals.
The Progression of Detachment
Once a retinal tear occurs, the detachment can progress rapidly. The liquefied vitreous can spread quickly, detaching larger areas of the retina. The longer the retina remains detached, the greater the potential for permanent vision loss. This is why prompt recognition and treatment are paramount.
Retinal detachment is a serious condition that can be particularly associated with high myopia, a refractive error that affects many individuals worldwide. Research indicates that those with high myopia are at a greater risk for developing retinal issues, including detachment, due to the elongation of the eyeball and changes in the retina. For more insights on this connection, you can explore a related article that discusses the implications of high myopia on eye health. Understanding these risks is crucial for early detection and prevention strategies. To read more about this topic, visit this informative article.
Recognizing the Warning Signs: What to Watch For
| Study | Findings |
|---|---|
| Eye (Lond) | High myopia is a significant risk factor for retinal detachment |
| Journal of Ophthalmology | Patients with high myopia have a higher incidence of retinal detachment |
| American Journal of Ophthalmology | High myopia is associated with an increased risk of retinal detachment |
The urgency of treating retinal detachment necessitates a keen awareness of its symptoms. Early detection significantly improves the chances of successful surgical repair and vision preservation.
Visual Disturbances: The Red Flags
The onset of certain visual symptoms can be indicative of a retinal tear or detachment. It’s vital to take these seriously and consult an eye care professional without delay.
Flashes of Light (Photopsia)
You might suddenly notice bright, flickering flashes of light, often in your peripheral vision. These flashes are typically described as being like lightning or camera flashes. They are often caused by the vitreous gel pulling on the retina, stimulating the photoreceptors. While flashes can occur with PVD, persistent or sudden onset flashes, especially when accompanied by other symptoms, should be investigated.
Floaters: New or Increased
You might observe new floaters – small specks, dots, or cobweb-like shapes that drift across your field of vision. These are caused by small debris within the vitreous humor. An increase in the number or size of floaters, particularly when they appear suddenly, can signify bleeding into the vitreous, which might be related to a retinal tear.
A Shadow or Curtain in Your Vision
This is perhaps the most concerning symptom. You might experience a dark shadow or curtain that gradually obscures part of your vision, typically starting from the periphery and moving inwards. This indicates that a section of your retina has detached and is no longer functioning. This symptom often signifies that the detachment is already progressing.
A Sudden Decrease in Vision
In some cases, particularly if the macula (the central part of the retina responsible for sharp, detailed vision) becomes involved in the detachment, you may experience a sudden and significant drop in your overall vision. This is a critical emergency.
Taking Action: Managing Your Risk and Seeking Care
Given the elevated risk, a proactive approach to your eye health is essential if you are highly myopic. This involves regular professional eye examinations and prompt attention to any concerning symptoms.
The Importance of Regular Dilated Eye Exams
For individuals with high myopia, routine comprehensive eye exams are not just for updating prescriptions. They are crucial for monitoring the health of your retina and optic nerve.
Ophthalmic Screening for Myopia
Your ophthalmologist will use specialized instruments to examine the structures of your eye. A key part of this examination involves dilating your pupils with eye drops. This allows for a wider view of your peripheral retina, where tears and lattice degeneration often occur. This examination is essential for detecting changes before they become symptomatic.
Early Detection of Retinal Changes
During these dilated exams, your eye doctor can identify early signs of retinal thinning, lattice degeneration, and even small tears that might not yet be causing any noticeable vision problems. Catching these issues early can allow for preventative treatments, such as laser photocoagulation or cryopexy, to be performed. These procedures can seal retinal tears and strengthen the retina to prevent detachment.
When to Seek Immediate Professional Attention
Do not delay in contacting your eye doctor if you experience any of the warning signs mentioned earlier. Time is of the essence when it comes to potential retinal detachment.
Prompt Referral and Diagnosis
If your symptoms warrant it, your ophthalmologist will likely refer you to a retinal specialist for further evaluation and, if necessary, treatment. The specialist will conduct a thorough examination using advanced diagnostic tools like optical coherence tomography (OCT) and ultrasound to confirm the diagnosis and assess the extent of the detachment.
Understanding Treatment Options
Treatment for retinal detachment usually involves surgery. The specific surgical approach will depend on the type and extent of the detachment. Common procedures include:
- Pneumatic Retinopexy: A bubble of gas is injected into the eye to help flatten the retina, often combined with laser or freezing treatment to seal tears.
- Scleral Buckle: A silicone band is placed around the outside of the eyeball to indent it and push the eye wall against the detached retina, helping to reattach it.
- Vitrectomy: The vitreous humor is removed from the eye, allowing the surgeon to directly access and repair the retina. This is often used for more complex detachments.
Lifestyle and Ongoing Care
While you cannot reverse your myopia or eliminate your increased risk entirely, there are steps you can take to support your overall eye health and potentially mitigate some risks.
Maintaining a Healthy Lifestyle
A healthy diet rich in antioxidants, omega-3 fatty acids, and vitamins can contribute to overall eye health. Maintaining a healthy weight and controlling conditions like diabetes and high blood pressure are also important, as these can indirectly affect eye health.
Avoiding Eye Trauma
While not always preventable, it’s prudent to take precautions to avoid direct trauma to your eyes. Wearing protective eyewear during sports or activities that pose a risk of eye injury is advisable.
Staying Informed and Vigilant
Continuously educating yourself about your eye condition and staying in communication with your eye care team is your best defense. Understand your specific risk factors, adhere to your recommended examination schedule, and never hesitate to report any new or developing visual symptoms. Your vision is a precious resource, and understanding the link between your high myopia and the risk of retinal detachment empowers you to protect it.
FAQs
What is retinal detachment?
Retinal detachment is a serious eye condition where the retina, the light-sensitive layer at the back of the eye, becomes separated from its normal position.
What is high myopia?
High myopia, also known as severe nearsightedness, is a condition where the eyeball is too long or the cornea is too curved, causing light to focus in front of the retina instead of on it.
How are retinal detachment and high myopia linked?
High myopia is a major risk factor for retinal detachment. The elongated shape of the eyeball in high myopia can lead to thinning of the retina, making it more prone to detachment.
What are the symptoms of retinal detachment in high myopia patients?
Symptoms of retinal detachment in high myopia patients may include sudden onset of floaters, flashes of light, or a curtain-like shadow over the field of vision.
How is retinal detachment in high myopia treated?
Retinal detachment in high myopia is typically treated with surgery, such as pneumatic retinopexy, scleral buckling, or vitrectomy, to reattach the retina and prevent vision loss. Early detection and treatment are crucial for a successful outcome.